Erectile Dysfunction
Erectile dysfunction (ED) is defined as trouble getting or keeping an erection that’s firm enough for sexual intercourse. Patients with ED may also experience other symptoms including premature or delayed ejaculation, low energy, being easily fatigued, and passiveness. According to the Urology Care Foundation, ED is the most common sex problem affecting as many as 30 million American men, about 50% of men over the age of 40. ED can occur from health problems such as physical conditions, emotional issues, or both.
A physical cause of ED can occur when there is not enough blood flow into the penis or when the parasympathetic and somatotropic nervous function is disturbed. This can occur due to many different health issues including the heart, hormones and the kidneys. Atherosclerosis, hardening of the arteries, can cause a lack of blood to the male sex organs through the narrowing of the arteries. The arteries that branch from the abdomen to the penis can be affected therefore causing the lack of blood flow. Vascular disease can cause ED in as many as 50% to 70% of men who have it.
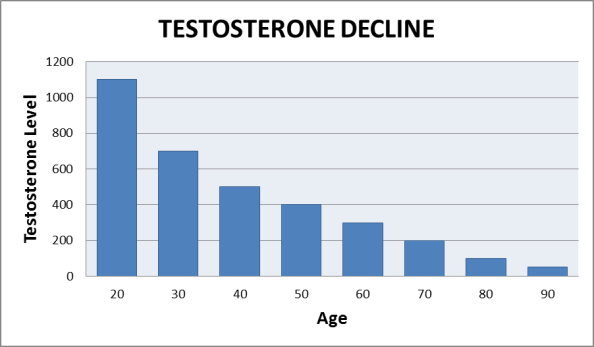
Testosterone is the key male sex hormone that regulates a number of processes in the male body including fertility, muscle mass, fat distribution and the development of male sexual characteristics. Testosterone levels decline with age and it has been viewed as the cause of ED. It is believed that ED can occur when testosterone levels drop below a certain threshold. When this threshold is reached, additional amounts do not further increase the frequency, amplitude, or rigidity of an erection.6
Testosterone has been widely used as an important therapy for ED. However, a more recent study has shown that testosterone replacement therapy is associated with heightened risk for kidney stones, according to an analysis of more than 50,000 men with low testosterone. Animal studies have suggested that testosterone replacement can increase oxalate and decrease citrate levels in the kidney, both of which may increase the risk of stone formation.8

Cortisol is a steroid hormone that regulates a wide range of vital processes throughout the body, including metabolism and the immune response. It also has a very important role in helping the body respond to stress. Cortisol levels rise with age after 40 years old. Research studies have shown that cortisol levels negatively correlate with erectile function. High cortisol levels can disrupt not only the male libido but can also cause erectile dysfunction. The negative effect of cortisol on erectile function occurs because cortisol narrows the arteries and causes blood flow restriction.5
The initiation, maintenance, and rigidity of a penile erection are under parasympathetic and somatotropic control. High cortisol levels activate the sympathetic nervous system which interrupts the parasympathetic and somatotopic activity. Sympathetic pathways are anti-erectile because the sympathetic nervous activity has a restraining effect on erections. Switching off the activity of the sympathetic nervous system enhances erections.7
Kidney diseases and adrenal deficiency can cause ED. ED is a common condition among male chronic kidney disease patients. Its prevalence is estimated to be approximately 80%. It is caused by the reduction of sex hormones in these patients.
Psychological factors are responsible for about 10%-20% of ED cases. The most common psychological causes of ED include stress, anxiety, and depression. Depression affects a person physically and psychologically. Depression can cause ED even when a man is completely comfortable in sexual situations.
Cortisol is a stress hormone released by the adrenal glands. Our brain triggers cortisol release in response to many different kinds of stress through the activation of the hypothalamic-pituitary-adrenal axis. When cortisol levels are too high for too long, it can cause ED. People with depression tend to have reduced levels of serotonin in the brain and elevated levels of cortisol in their bloodstream. Besides emotional stress, the stress from chronic diseases such as diabetes, high blood pressure, Parkinson’s, cancer, injury or surgery can also cause elevated cortisol levels. Smoking, alcohol, drugs, and many prescription medications can also cause a cortisol level increase and heighten the risk of ED.
Stress and anxiety can also interrupt how the brain sends messages to the penis and interrupts blood flow. Experiencing ED can cause further stress and lead to behavioral changes that can further aggravate ED.
Post-traumatic stress disorder (PTSD) has shown to cause hypersensitivity of cortisol receptors which augment the effect of cortisol. A study with veterans who suffered from post-traumatic stress disorder (PTSD) showed that PTSD increased the risk of sexual dysfunction by more than three times.4
Prostate Enlargement
Prostate enlargement, known as benign prostatic hyperplasia (BPH), is a condition in which the prostate gland becomes enlarged and can cause uncomfortable urinary symptoms. BPH is mainly caused by the proliferation of smooth muscle and epithelial cells located in the prostate.
The symptoms of BPH include urinary frequency, urinary urgency, an interrupted and weak urine stream, nocturia, urinary retention, and pain after ejaculation or urination. These symptoms arise from a blocked urethra and/or an overworked bladder.
Although the etiology of BPH is unknown, testosterone and dihydrotestosterone (DHT) are well-known to be related to the development of BPH. As men age, the amount of active testosterone in the blood decreases. Serum testosterone has been shown to decrease in men with age by approximately 2%–3% annually. Testosterone is produced in the testes and then spreads to the prostate where it is converted into dihydrotestosterone (DHT) through an enzyme, 5α-reductase (5AR). DHT is an endogenous androgen sex hormone responsible for prostate development. While testosterone decreases with age, the activities of 5AR and androgen receptors (AR) are increased due to androgen balance.1 In BPH patients, shared common features consist of proliferated prostate cells and increased DHT, AR, and PSA levels. High concentrations of DHT enhance prostate-specific antigen (PSA) levels by binding with the androgen receptors. PSA levels increase when the prostate is inflamed and is how prostate inflammation is monitored through blood tests (normal range <4.0 ng/ml, and <2.5 ng/ml for men under 50).
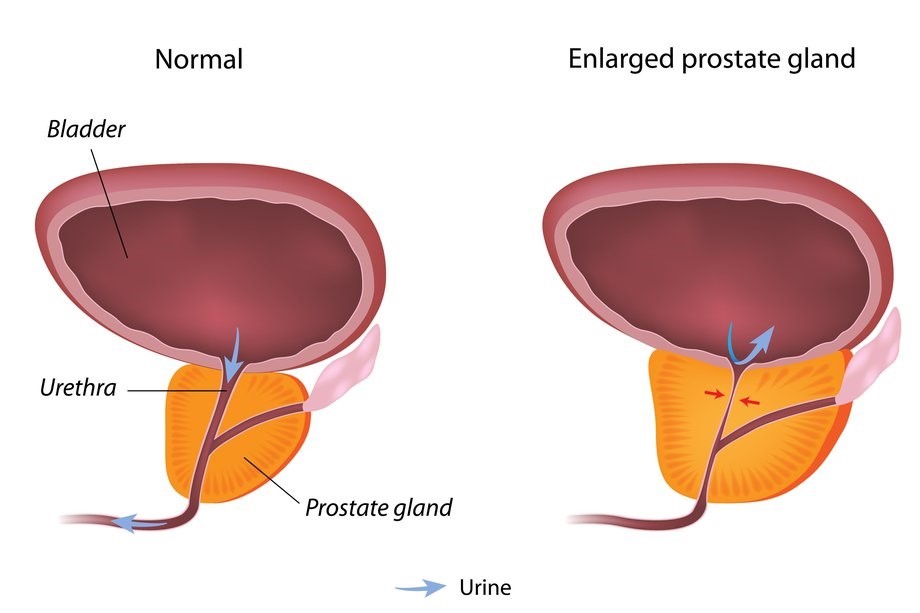
Testosterone replacement therapy has been widely used as a treatment for ED. Since research has confirmed that prostate growth is proportional to testosterone levels, FDA has mandated warning on all testosterone products and stated that testosterone replacement therapy (TRT) in men with benign prostate hyperplasia (BPH) increases the risk of worsening signs and symptoms of BPH.
Estrogen is also found in the prostate and can contribute to the development of BPH. Estrogen receptors such as estrogen receptor-α (ERα), within the prostate, can mediate cell proliferation, whereas, estrogen receptor-ß (ERß) mediate apoptosis (programmed cell death).1 Aromatase is located in estrogen-producing cells in the testes and is involved in the production of estrogen by converting testosterone to estradiol. Estradiol binds with ERα where it enters into the nucleus and acts as a transcription factor which results in proliferation of the prostate cells.1
Kidney and bladder damage and infection can occur and cause urinary tract inflammation in BPH patients due to the interruption in urine flow and urine retention. The urinary tract inflammation can further affect the prostate and aggravated prostate inflammation causing a further increase of the PSA levels.
Male Infertility
About one-third of infertility cases are caused by male infertility. Male infertility is caused by low sperm production, abnormal sperm function, or blockages that prevent the delivery of sperm. In TCM, male infertility can be linked to a kidney deficiency, a liver qi stagnation, a deficiency in qi, and blood stasis. Any one of these can cause a decrease in sperm quality. Sperm quality is measured by several different factors that include the production of healthy sperm, transportation of sperm into semen, quantity of sperm in the semen, and sperm motility.
Symptoms of male infertility include the inability to conceive a child and in some cases, is the only symptom. Others can also experience hormonal imbalances, erectile dysfunction, pain or swelling in the testicles, abnormal breast growth, decreased facial or body hair, or low sperm count (fewer than 15 million sperm per mL of semen).
A kidney deficiency, in TCM, is the fundamental pathogenesis of male infertility. It has been shown that a kidney deficiency often coincides with an impaired structure of the hypothalamic-pituitary-testicular (H-P-T) axis1. The H-P-T axis is an important part of the endocrine system that regulates testicular function. Many experiments have shown that formulas that support the kidneys could repair the structure and restore the function of the H-P-T axis and regulate hormone levels to increase the level of testosterone and improve the quality of semen.1
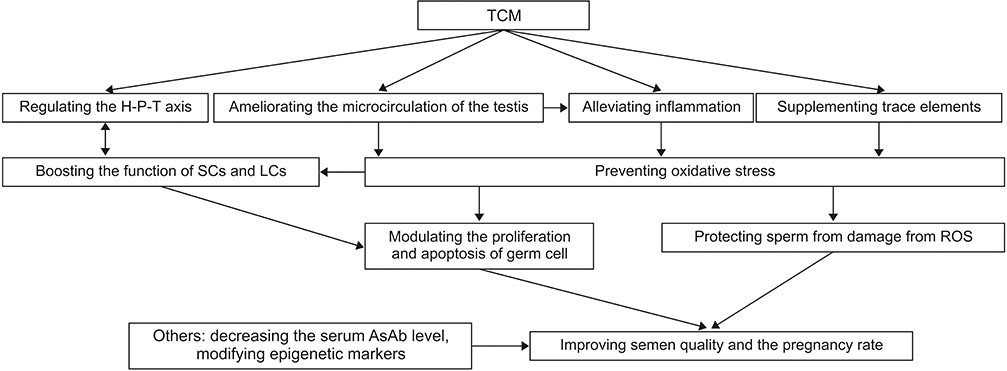
Fructus Lycii, an herb found in Wei Labs MI Formula, has been shown to increase follicle-stimulating hormone (FSH) and luteinizing hormone (LH) in rats.2 FSH and LH are both gonadotropins which stimulate the gonads and increase testosterone production. Fructus Lycii also has been shown to increase superoxide dismutase levels and reduce malondialdehyde in the testes to protect sperm from oxidative stress.3 Oxidative stress causes cellular damage and can attack the membrane of the sperm cells leading to decreased fluidity.